Table of Contents
There are several possible locations for sural neuropathy. The fifth metatarsal base is a frequent location for this condition. The sural nerve has a bifurcation, with medial and lateral terminal branches, and leaves the crural fascia. If the pain in this area is accompanied by weakness or tenderness, it can be indicative of a neuropathic condition. Treatment options vary widely depending on the cause.
MRI
MRI is a useful diagnostic tool in evaluating patients who have symptoms of sural nerve pain. The study uses magnetic resonance imaging (MRI) to visualize compression, displacement, and space-occupying lesions of the sural nerve. Sural nerve pain is not usually a severe case, and there is no evidence of denervation, although the study can help identify whether a previous injury or surgery has affected the nerve.
An MRI may be needed to rule out other possible problems. Sural nerve pain is often difficult to diagnose because the symptoms do not show up on x-rays. While MRI can rule out other issues, it does not reveal the underlying cause of the problem. MRI does have a few advantages. First, it can rule out other potential causes of sural nerve pain, including spinal fracture, tumor, or infection.
A 72-year-old woman presents with anterolateral knee pain for 2 months and has undergone medial patellofemoral ligament reconstruction. She has a history of sural nerve biopsy. On axial proton-density MR images, she has a neuroma-in-continuity of the saphenous nerve. On the other hand, on preoperative MR images, she had a full-thickness transection of her sural nerve, resulting in a 2.2-cm gap. Moreover, her Achilles tendon is also gapped.
Acute or chronic pain originating from the sural nerve is referred to as sural neuritis. Patients with the symptoms of sural nerve pain may also experience complex regional pain syndrome (CRPS), a debilitating condition characterized by severe leg pain and intractable ankle dysfunction. This condition may be easily treated with conservative measures or surgical interventions. It is best to consult a specialist if your symptoms persist after conservative measures have been unsuccessful.
Acute or chronic entrapment of the nerve may cause sural nerve pain. If the nerve is inflamed, it will show changes in morphology and signal intensity. The affected nerves will become flat and enlarged at the entrapment site, and may also exhibit hypointense or hyperintense signal on T2W images. There may also be effacement of the perineural fat. An MRI along the long axis of the nerve will also show changes in the muscles innervated by the affected nerve.
Diagnostic nerve blocks
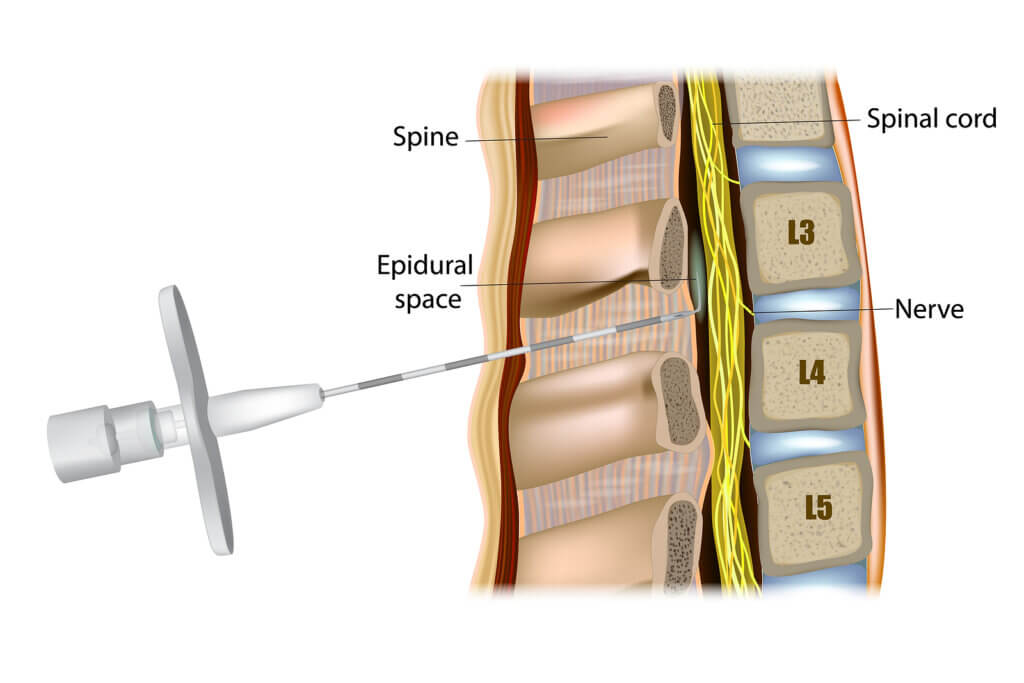
A diagnostic nervous block of the sural nerve is used in cases where pain in the ankle, heel, or foot is persistent and not responsive to rest or medication. It can also be used during surgery for conditions that involve the sural nerve, such as bunionette surgery. Diagnostic nerve blocks for sural nerve pain are often combined with peripheral nerve blocks to target a larger area of the foot and ankle. For more information, talk to your doctor about your options.
An effective sural nerve block is an alternative to spinal anesthesia. In recent years, many surgeons have begun using sural nerve blocks for the treatment of chronic hemiplegic shoulder pain in patients with chronic stroke. However, well-designed studies are needed to verify these results. This technique is not appropriate for patients with severe chronic pain. Consequently, it should not be used as a primary therapy for chronic pain.
Various procedures can be performed to block the pain coming from the sural nerve. These include a single-injection technique, which involves injecting a local anesthetic into a small nerve and then leaving the area for a short period of time. Another common technique is a continuous peripheral nerve block, which involves a percutaneous insertion of a catheter near the targeted nerve. This procedure usually provides a prolonged period of analgesia and can be performed as an outpatient procedure.
Patients with chronic headache may undergo diagnostic nerve blocks for sural nerve pain. These procedures can help reduce the intensity and frequency of occurrence of these symptoms. Among the other treatments, they are also effective for the treatment of primary or secondary cluster headache. Diagnostic nerve blocks are most often performed using local anesthetics (amide-type local anesthetics).
During a diagnostic nerve block, the surgeon can visualize the sural nerve at the ankle level. Typically, the patient lies prone on the operating table with the ankle everted. This position places the foot at a 90-degree angle to the leg. The lesser saphenous vein becomes distended when the calf is compressed and can be identified in the trough between the Achilles tendon and external malleolus. This vein is the best anatomic landmark for the sural nerve.
Treatment options
Surgical interventions can provide relief for sural nerve pain. Sural nerve decompression can be done under local anaesthesia by cutting a longitudinal segment of the fascial tunnel and releasing the sural nerve from fibrous tissue. This procedure may also involve long proximal dissection. If conservative measures are not enough, a combination of surgical and non-surgical procedures may be recommended. Patients can expect to feel numbness along the nerve's course following the procedure.
X-rays and MRIs are inconclusive for this condition, but newer, cheaper ultrasound techniques have made these procedures more useful. A scan can also rule out other problems. Non-surgical treatments include direct massage to the nerve and physical therapy. Surgical techniques may also be necessary to free the nerve from scar tissue. The goal of treatment is to alleviate pain and restore mobility to the affected area.
Sural nerve neuropathy may result in other painful conditions, such as complex regional pain syndrome. Treatment of sural neuritis must include treatment of underlying conditions. However, surgery may be necessary for more severe cases. Patients with sural nerve pain should discuss their condition with their doctor before undergoing any surgery. This is because surgical interventions can be a dangerous option for the nerve. In addition to surgery, conservative measures may be necessary to treat sural neuritis.
Nonsurgical treatment options include biomechanical and postural corrections. The clinician should be mindful of repetitive movements that may irritate the nerve. Non-steroidal anti-inflammatory medications and steroid injections may also be necessary. Physical therapy can also be prescribed to alleviate pain and restore function. EMG testing may be necessary to diagnose the cause of sural nerve pain. EMG testing is more accurate than testing over the skin.
Ankle sprains may occur in an untreated or recurrent sural nerve. Such injuries force the joint out of its natural position, causing the sural nerve to become compressed. Athletes may experience ankle sprains or fractures. Other sports injuries that may cause sural nerve pain include wearing tight shoes and ankle straps. Some surgical procedures may result in space occupying lesions and compression of the sural nerve.
Common causes
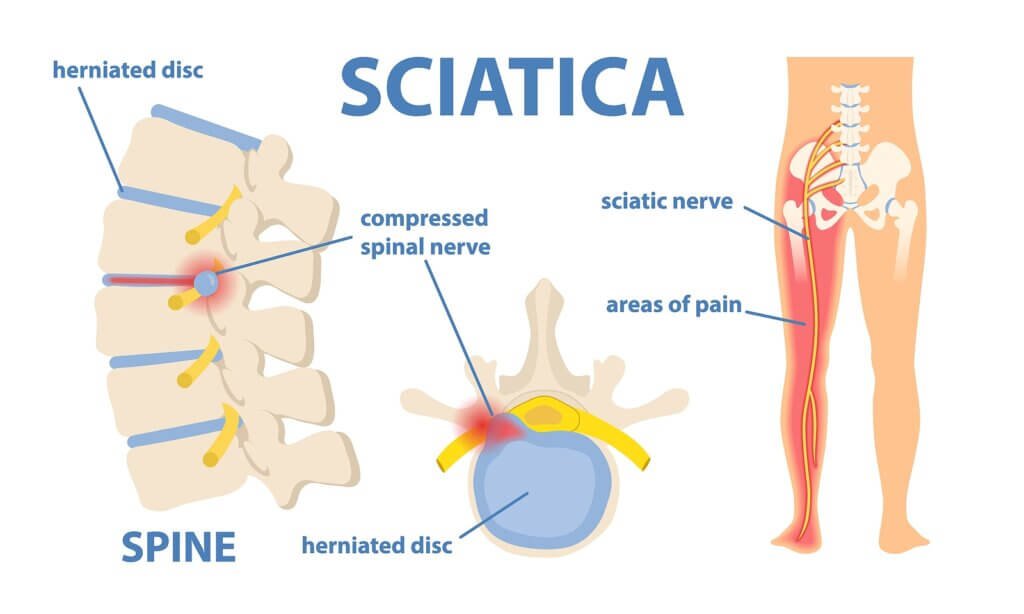
There are several common causes of sural nerve pain. These include trauma, exercise, musculoskeletal problems, and compartment syndrome. There are other causes of leg pain, such as nerve entrapment. Let's look at a few of these common causes. The most common one is trauma. Listed below are some of them. You may also experience leg pain when walking or running. However, it's important to seek medical attention immediately if you notice pain in your leg.
Sural nerve damage can be a symptom of other underlying conditions, such as a spinal cord injury. There are three main types of nerves. The sensory nerves pick up and send sensory signals, while motor and sensory-evoked neurons process electrical impulses. Damage to these nerves can lead to paralysis and other conditions. It can also lead to complex regional pain syndrome. This condition can be very debilitating.
Treatment for sural nerve pain usually involves addressing the underlying cause of the injury. Direct message may be performed to desensitize the nerve and break up the scar tissue around it. While desensitization may be uncomfortable at first, the pain will subside with time. Other treatments include physical therapy and injections. If conservative treatments fail, sural nerve neuropathy may need surgery. Your doctor will discuss the options with you.
The most common causes of sural nerve pain are traumatic injuries and entrapment. Various causes of sural nerve pain may occur, including acute trauma and entrapment within scar tissue. Chronic traction injuries may also cause sural nerve pain. In the worst cases, it can be due to a nerve injury. Depending on the underlying cause, treatment may involve medications, corticosteroids, or aggressive massage. In extreme cases, surgery may be necessary to release the scar tissue or excise the damaged nerve.
Surgical treatment for sural nerve pain involves decompression of the sural nerve. This procedure is performed under local anesthesia. It involves cutting a longitudinal section of the fascial tunnel to free the sural nerve from fibrous tissue. Sometimes, a long proximal dissection is necessary. If you don't find relief with these methods, see a doctor for more information. Your doctor will recommend the appropriate course of treatment based on the condition and the severity of the pain.



Comments
Loading…