Whether you're experiencing genitofemoral or ilioinguinal nerve pain, you can find relief through a variety of treatment options. Learn more about the diagnosis and treatment of this type of pain. Listed below are some of the most effective and current pain management options available in the USA. For more information about these options, visit our website. Also, find out more about pain management in general.
Treatment options for ilioinguinal nerve pain
A common source of lower abdominal pain, the ilioinguinal nerve emerges from the lumbar spinal nerves in the lower back. The nerve travels down the inner thigh, groin, and perineum, providing sensation and pain to the surrounding area. An injury to the lower back or muscle can damage the ilioinguinal nerve, causing pain in the groin, inner thigh, or lower abdomen.
Conservative treatment may be ineffective, but nerve blockade and surgical neurectomy are both available. In the event of failed conservative methods, surgeons may decompress the nerve using a small injection. Surgical decompression is performed under ultrasound guidance, and results may take up to four weeks. This procedure is generally performed in an outpatient setting and requires a stay in the hospital for one to three days.
Hernia surgery can lead to a permanent nerve injury, which may cause a variety of symptoms, including pain and loss of quality of life. While the pain may improve after abdominal surgery, there is a significant risk of permanent damage. The damage may affect the patient's ability to walk, sit, or stand. Treatment options for ilioinguinal nerve pain can include surgery and medication.
In cases of chronic groin pain, medications can be used to relieve the condition and reduce or eliminate the symptoms. Noninvasive nerve blocks may be effective and may include acupuncture or transcutaneous electrical nerve stimulation. In some cases, local anesthetics are used to block neuronal transmission, block membrane ion channels, and denature axon proteins. A doctor's assessment and diagnosis of ilioinguinal neuralgia is important to determine the best course of treatment.
Opioids are the most commonly used pain medications for ilioinguinal nerve. SSRIs (selective serotonin reuptake inhibitors) work by blocking the activity of dopamine in the brain. Opioids are injected into the abdomen and can produce unpleasant side effects like sleepiness, constipation, and nausea. A doctor may prescribe a nonopioid medication like Dilaudid to relieve the pain.
Surgical interventions to repair an inguinal hernia are some of the most common causes of ilioinguinal nerve pain. Other possible causes of ilioinguinal nerve pain include tumors in the abdomen and spinal cord problems. These procedures can be very painful and can affect a person's life. Surgical treatment can be effective, but only if it is done by a qualified doctor.
The traditional anterior approach is an excellent choice for people suffering from ilioinguinal nerve pain, with a success rate of up to 90%. Surgical procedures are risky, and patients should be carefully evaluated for complications before proceeding with surgery. The best method is an interprofessional approach. A surgeon can minimize the risk of injury by utilizing a mesh that does not induce fibrotic reactions. Other healthcare professionals may be involved in the care of patients, such as physical therapists, nurses, and pharmacists.
Treatment options for genitofemoral nerve pain
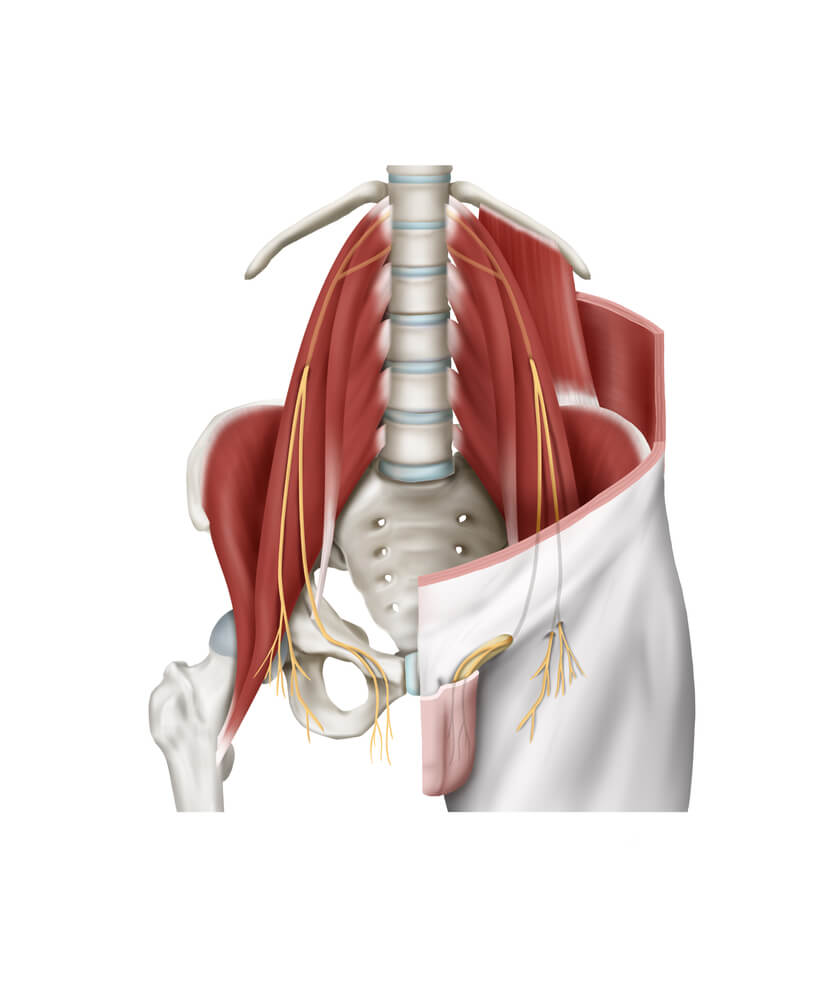
When an individual is experiencing pain in their lower abdomen, it is possible to suspect a condition called genitofemoral neuralgia. These symptoms include numbness, tingling, and burning over the lower abdomen and can radiate to the labia majora or scrotum. If left untreated, the pain can worsen and even cause bulging of the anterior abdominal wall muscles.
When pain persists and doesn't improve with conservative measures, it is a good idea to visit a doctor for a diagnosis. During pregnancy, the uterus places pressure on this nerve, which can aggravate its symptoms. Treatment options for genitofemoral nerve pain include spinal manipulation, nerve blocks, and medications. If the pain is persistent or is not going away, a doctor may recommend a visit to a specialist.
Although oral medications may offer temporary relief, genitofemoral nerve block injections are the preferred treatment for genitofemoral neuralgia. This minimally-invasive procedure involves injecting a local anesthetic and anti-inflammatory steroid into the affected nerve. The injection is effective in blocking the nerve and preventing pain signals from spreading throughout the body. This type of surgery is usually performed under image guidance.
In some cases, trauma can cause nerve damage, but if the injury is not severe, there are other treatment options. Inguinal hernia or pelvic surgery can cause damage to this nerve. These types of injuries are considered more serious and need a higher level of care. But whatever the cause, a doctor can offer you an effective treatment option for genitofemoral nerve pain.
An MRI may be performed to rule out tumors and masses. Depending on your medical history, additional tests may be ordered, such as x-rays and MRIs. Your doctor will likely recommend physical therapy if you experience this kind of pain. But remember: this article is not intended to provide medical advice. If you suspect you're suffering from genitofemoral nerve pain, please seek immediate medical help.
Ultrasound-guided GF nerve block is one of the most effective treatment options for genitofemoral neuralgia. It allows for precise localization and can also help rule out other nerves. There are a few case reports involving patients treated with this nerve block. However, the article aims to educate the reader on the diagnosis and treatment options of genitofemoral nerve pain.
Surgical treatments for genitofemoral nerve pain are available. The genital branch of the GF nerve is the most commonly affected. Surgical procedures involve the incision of the pubic tubercle, and a 1.5-inch, 25-gauge needle is inserted through it. Once the needle has contacted the fascia of the external oblique muscle, 2.5 mL of bupivacaine is injected.
Identification of ilioinguinal nerve pain
Various causes of ilioinguinal nerve radiculopathy include surgery for inguinal hernia, tumors of the abdominal organs, and abdominal trauma. Occasionally, spinal cord problems may also cause pain in the ilioinguinal region. Patients suffering from chronic groin pain should seek medical attention for the condition. This article focuses on the identification and treatment of this disorder.
Identifying ilioinguinal neuralgia is crucial to providing the best possible treatment and care. The interprofessional approach is beneficial for improving prognosis. The interprofessional team may collaborate to address pain management options. The patient can learn from his or her therapists about a healthy lifestyle, and the pharmacist can provide information about the available pain medications. A physician can also refer the patient to a neurologist if the condition persists.
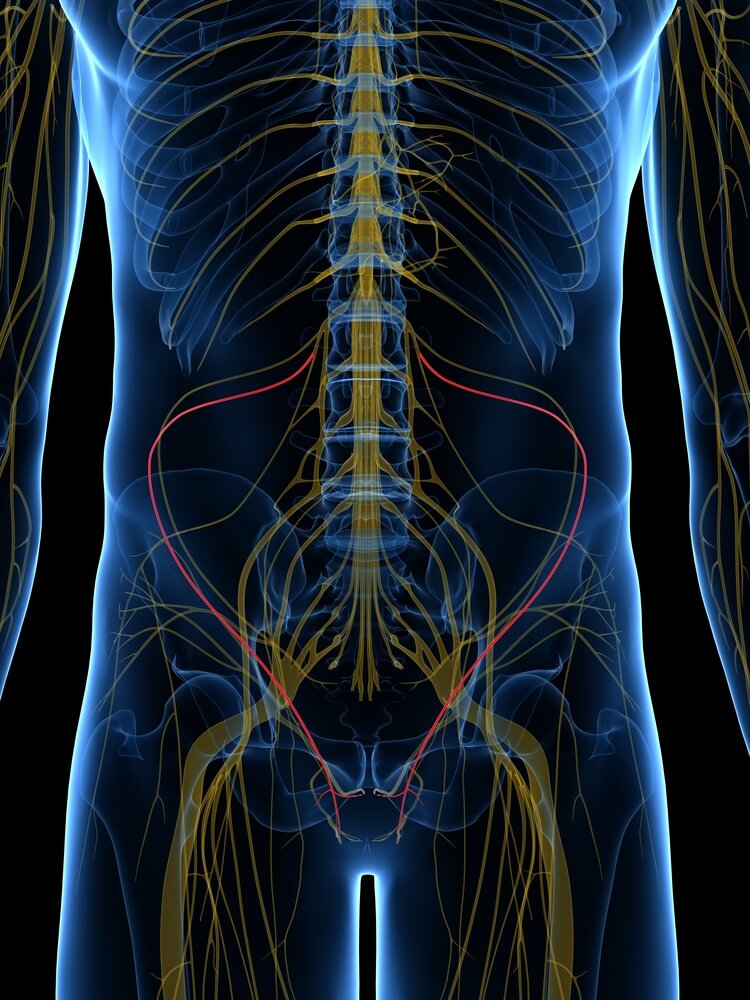
If you experience chronic pain in the lower abdomen, it may be caused by ilioinguinal nerve radiculopathy. This condition involves pain in the groin and lower abdomen. It originates from the spinal cord and travels through the anterior abdominal wall to innervate the genital organs. The pain often radiates to the genital region, lower abdomen, and inner thigh.
Surgery to identify the ilioinguinal nerve is a common procedure to alleviate chronic ilioinguinal nerve radiculopathy. This procedure involves a small injection that relieves pain. Although the surgery is invasive, it reduces the occurrence of postoperative pain caused by nerve injury. Further, this technique is effective in reducing the risk of complications from nerve injuries.
An ilioinguinal nerve block may be effective in reducing the pain in groin areas. A local anesthetic mixed with an inflammation-reducing steroid is injected around the ilioinguinal nerve. Image guidance may be used to enhance the accuracy of the procedure. Despite the risk of infection, this procedure has helped many patients overcome chronic pain. If the neuroma is causing you chronic pain, you should consult a physician.
A recent study found that inguinal hernioplasty may cause persistent postoperative groin pain. While most of the patients report mild or moderate groin pain, it can be incapacitating and interfere with daily activities. Consequently, the goal of this research is to identify the causes of ilioinguinal nerve pain. The goal is to prevent postoperative neuropathies and to reduce the risk of permanent damage.

Comments
Loading…